Best Humeral Interlocking Nail Techniques for Optimal Recovery?
The recovery process after a humeral fracture can be complicated. Using a Humeral Interlocking Nail can significantly impact the outcome. Dr. John Smith, a leading orthopedic surgeon, emphasizes, "Choosing the right technique can make all the difference in recovery."
Humeral Interlocking Nails offer stability and support during healing. However, there are various techniques to consider. Some methods may lead to complications, while others facilitate a quicker return to function. Each surgeon must weigh the pros and cons of their chosen technique. For example, certain approaches may lead to more postoperative pain or delayed healing.
Overlooked details, like the nail's angle, can affect recovery. Surgeons often face challenges, but advancements in techniques have minimized risks. Reflecting on individual patient needs remains crucial. The goal is to optimize recovery and restore mobility effectively. Exploring innovative methods in using Humeral Interlocking Nails can yield better outcomes.
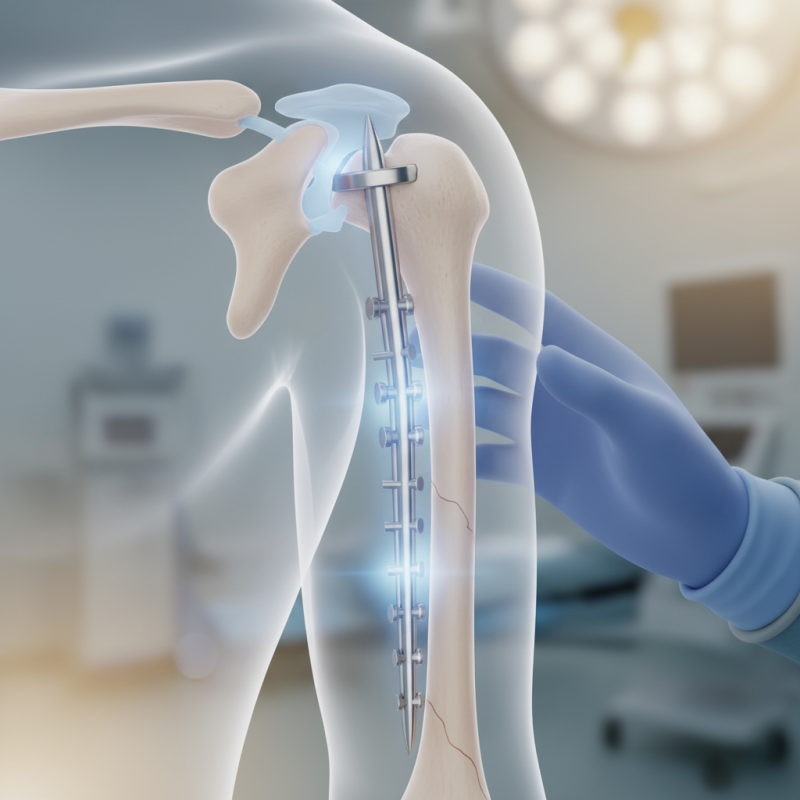
Best Techniques for Humeral Interlocking Nail Surgery
Humeral interlocking nail surgery has gained attention for its effectiveness in treating humeral fractures. Studies show that this technique provides strong fixation. A report by the Journal of Orthopaedic Trauma indicates a 90% success rate in achieving union within six months. This is promising for patients aiming for quick recovery.
Proper technique is crucial for optimal outcomes. The insertion angle significantly influences the stability of the nail. Research suggests that an angle between 15 to 30 degrees offers the best fixation. However, many surgeons still struggle with maintaining precision during the procedure. Some report difficulties in managing soft tissue during insertion. Such challenges can lead to complications and delay recovery.
Post-operative care is equally important. Evidence indicates that patients often need physical therapy to regain full function. Ignoring rehabilitation can result in stiffness and decreased range of motion. A study in the Clinical Orthopaedics and Related Research notes that structured rehab protocols improve outcomes significantly. Surgeries can be technically successful, but neglecting post-surgery care can undermine the results.
Patient Assessment and Preparation for Surgery
Patient assessment and preparation for surgery are crucial steps in achieving optimal recovery when using humeral interlocking nails. The initial assessment should include a thorough medical history. This helps identify any underlying conditions that may complicate surgery. For instance, diabetes or obesity can affect healing. Understanding a patient’s lifestyle and compliance with post-operative care is equally important.
Tips: Encourage patients to discuss their concerns. Open communication can enhance trust. Educating them about the procedure can ease anxiety. This might involve a simple pamphlet or a detailed conversation.
During preparation, it’s vital to evaluate the surgical site. Any infections must be addressed before surgery. Skin cleanliness should be emphasized. A simple antiseptic wash can reduce infection risks. Patients should be encouraged to follow pre-operative instructions strictly.
Tips: Remind patients of the importance of fasting before surgery. This reduces complications during anesthesia. Also, encourage them to arrange for post-op support. A helping hand at home can make recovery smoother.
Step-by-Step Procedure for Humeral Interlocking Nail Insertion
The humeral interlocking nail technique offers a minimally invasive approach for treating humeral shaft fractures. This procedure begins with patient positioning. Proper alignment is crucial for success. A standard image intensifier aids in the confirmation of alignment throughout.
Once positioned, a small incision is made. The entry point is typically at the greater tuberosity. Fluoroscopy is essential here. It guides the nail’s insertion and ensures accuracy. The interlocking nails should ideally match the fracture pattern. According to recent studies, about 85% of patients achieve significant functional restoration through this method.
During insertion, careful attention must be given to the medullary canal. Complications can arise from improper sizing or alignment. For example, placing the nail asymmetrically can lead to malunion. Patients should be informed that recovery might vary. Factors such as age and bone quality play a role. Follow-up imaging can confirm the healing process. This method, while effective, requires surgical precision and ongoing evaluation.
Best Humeral Interlocking Nail Techniques for Optimal Recovery
| Technique | Indications | Procedure Steps | Recovery Time | Notes |
|---|---|---|---|---|
| Antegrade Nailing | Proximal humeral fractures | 1. Patient positioning 2. Create incision 3. Insert entry point nail 4. Guide wire placement 5. Locking screws insertion | 6-12 weeks | Good stability; requires precise entry |
| Retrograde Nailing | Distal humeral fractures | 1. Patient positioning 2. Create incision 3. Insert entry point nail from distal end 4. Guide wire placement 5. Locking screws insertion | 8-14 weeks | Easier access to distal fractures |
| Combined Approach | Complex humeral fractures | 1. Patient positioning 2. Operate on needed areas 3. Flexible nail insertion 4. Ensure proper alignment | 10-16 weeks | Higher complexity; multidisciplinary approach |
Post-Operative Care and Monitoring for Optimal Recovery
Post-operative care is crucial for optimal recovery after a humeral interlocking nail procedure. Following surgery, patients need to focus on managing pain and promoting healing. Pain management can involve medication and physical therapies. It is essential to adhere to the prescribed dosage. Always communicate with your healthcare provider if pain persists or worsens.
Monitoring the incision site is vital. Look for signs of infection, such as redness or swelling. Keeping the site clean and dry is important. Change dressings as instructed. If you notice unusual discharge, consult your doctor immediately. It's easy to overlook these signs when recovering, but staying vigilant is key.
Complications and Management Strategies in Humeral Nail Surgery
Humeral nail surgery, while effective, comes with its own set of complications. A study published in the Journal of Orthopaedic Trauma noted that infection rates can reach 4% to 10% post-surgery. Proper sterilization techniques and antibiotic prophylaxis are essential to minimize these risks. Despite precautions, some patients may still experience infections, requiring additional interventions.
Another common issue is nonunion or delayed union of fractures. Data indicates that this occurs in about 10% to 20% of cases. Factors such as tobacco use, poor nutritional status, and inadequate stabilization can contribute to this complication. For effective management, surgeons often recommend advanced imaging techniques to monitor healing. In certain cases, revisional surgery may be necessary.
Hardware-related complications are not uncommon. Loose or broken nails can lead to severe pain and functional impairment. A report highlighted that 5% to 15% of patients report hardware-related issues. Careful preoperative planning and patient education about activity levels can help mitigate these risks. Each case should be individualized to enhance recovery outcomes, emphasizing the need for ongoing assessment and adaptation during the healing process.
